🎁 Welcome to The Byte 2.0!
The Byte is The AI Collective’s leading publication for thought leaders sharing about the incredible discoveries they’ve made and projects they are working on.

In this week’s edition of The Byte, Kiran Suryadevara and Audrey Kennedy explore the rise of medical superintelligence. From ambient sensing and wearable-derived movement data to the biochemical frontier of volatile organic compounds, they examine how multimodal AI systems are shifting healthcare from episodic snapshots to persistent, personalized baselines capable of detecting disease years before symptoms appear. Lastly, they also confront the regulatory and ethical trade-offs of a world where our bodies constantly emit signals that technology can interpret.
For more information or how to get in touch with The Byte editorial team, send us a message at [email protected].
~ Josh Evans, Managing Editor
Snapshots to Signals: The Data Powering Medical Superintelligence
In an era defined by performance optimization, sensor technology has brought the universal promise of better health to the masses, offering a constant stream of insights into how we sleep, move, metabolize, and recover. Even as AI systems have expanded and accelerated data processing, healthcare is still built on episodic snapshots of our physiological, behavioral, and environmental states, each one captured in isolation and stitched together by clinicians trying to reconstruct a patient’s journey.
A new phase is now emerging: medical superintelligence. These are multimodal systems that read the body as a continuous, dynamic process unfolding in real time, moving medicine from occasional check-ins to a persistent understanding of how the body evolves in daily life and contextualizing the rhythms and deviations that define real-world health. Put simply, medical superintelligence is what happens when all our scattered health signals finally start speaking the same language. We’re already seeing this in practice.
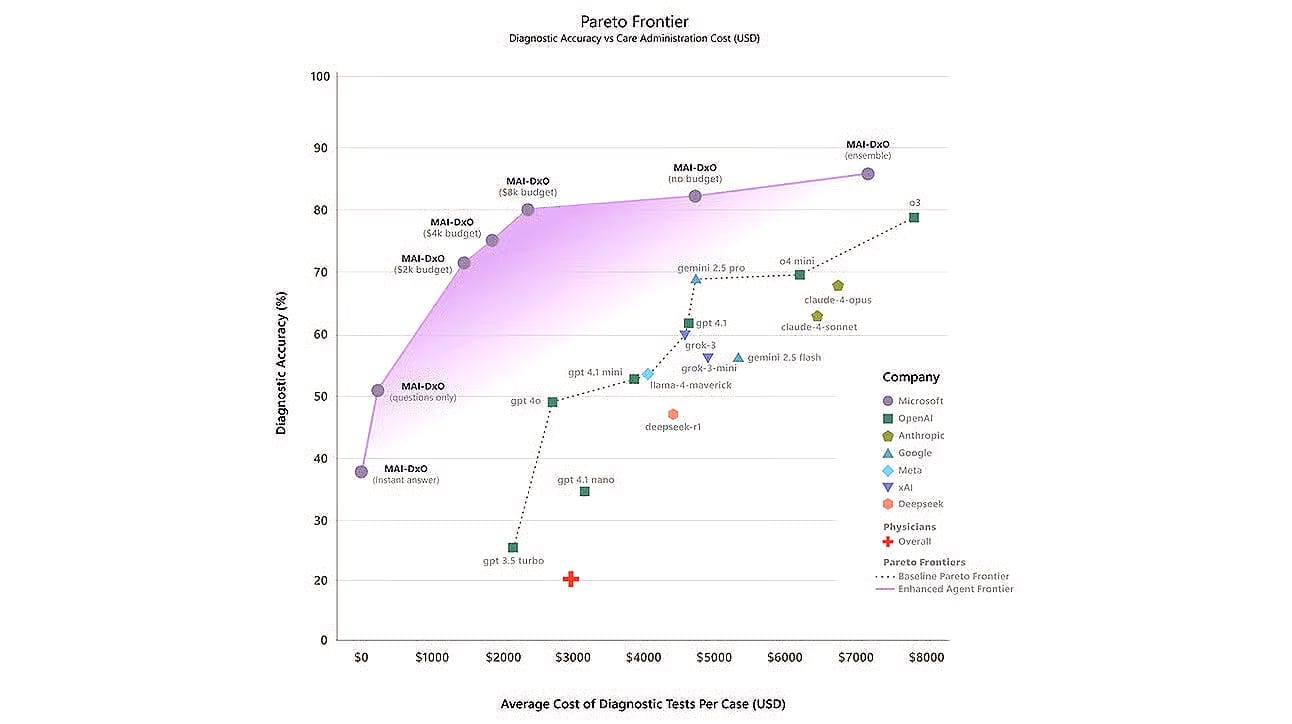
Figure 1. Diagnostic Accuracy vs Care Administration Cost (USD). “The Path to Medical Superintelligence”
Towards the end of last year, Microsoft introduced its Medical AI Diagnostic Orchestrator (MAI-DxO), an early attempt to create a unified reasoning layer. Cloud strategy is increasingly becoming clinical strategy, with the control points of healthcare now shifting toward unified data platforms and model-orchestration layers that allow AI systems to run, update, and reason inside clinical workflows.
AI enables the creation of individualized health baselines and the detection of subtle changes long before symptoms emerge, whether it is a slight rise in resting heart rate days before illness, small shifts in gait that signal fall risk, sleep fragmentation that precedes depressive relapse, or recovery patterns that fluctuate with stress and travel.
This is the direction people are starting to refer to as medical superintelligence. It is not a single model, but an emerging intelligence layer designed to sit between observed health and the institutions that act on it. Its role is to integrate streams across physiology, behavior, and environment, translate them into clinically meaningful representations, and support reasoning within medical workflows. In other words, it is where what is sensed on and around the body begins to shape how care is actually delivered.
Health data is no longer limited to what is recorded in a chart. It increasingly includes what can be inferred from how we live and how our biology responds. And the most transformative shifts will come from modalities most of us do not even realize we are emitting. Two frontiers in particular are beginning to redefine how health is sensed and interpreted: ambient sensing and the biochemical analysis of volatile organic compounds (VOCs).
One of the key enablers of medical superintelligence is sensor technology, not because sensors are simply becoming smaller or more wearable, but because they are becoming ambient. Rather than relying on isolated snapshots of health data, ambient sensing captures continuous information through devices and spaces we occupy regularly: watches, rings, phones, smart fabrics, surface-based sensors, and environmental monitors.

Figure 2. Ambient and localized sensing for passive physiological signal extraction. “Ambient health sensing on passive surfaces using metamaterials,”
Signals such as sleep quality, heart rate, movement patterns, breathing rhythms, and air quality may seem routine on their own, but when analyzed by machine learning, these data streams can reveal early warning signals of disease. For example, tracking and treating Parkinson’s disease present long-standing clinical challenges historically dependent on periodic clinic visits, where patient evaluations are often shaped by external factors and constrained by limited windows of observation.
A landmark study at Cardiff University demonstrated that machine learning applied to just one week of movement data from wearables identified individuals who would develop Parkinson’s disease up to seven years before clinical diagnosis, outperforming genetic testing, blood biomarkers, and conventional symptom screening. These advancements in sensor technology fundamentally shift the paradigm from reactive diagnosis to proactive risk identification, enabling intervention when treatments might actually prevent disease progression.
While ambient sensor systems primarily capture motion, temperature, pressure, and biophysics to monitor behavior, the next frontier is understanding the body’s biochemistry. Breakthroughs in biochemical research, especially the study of volatile organic compounds (VOCs), offer this deeper molecular layer. VOCs are small chemicals continuously emitted from our breath, skin, and sweat. They shape much of what we perceive as odor, but more importantly, they reflect underlying metabolic processes: inflammation, oxidative stress, digestion, infection, and in some cases, the earliest indicators of disease.
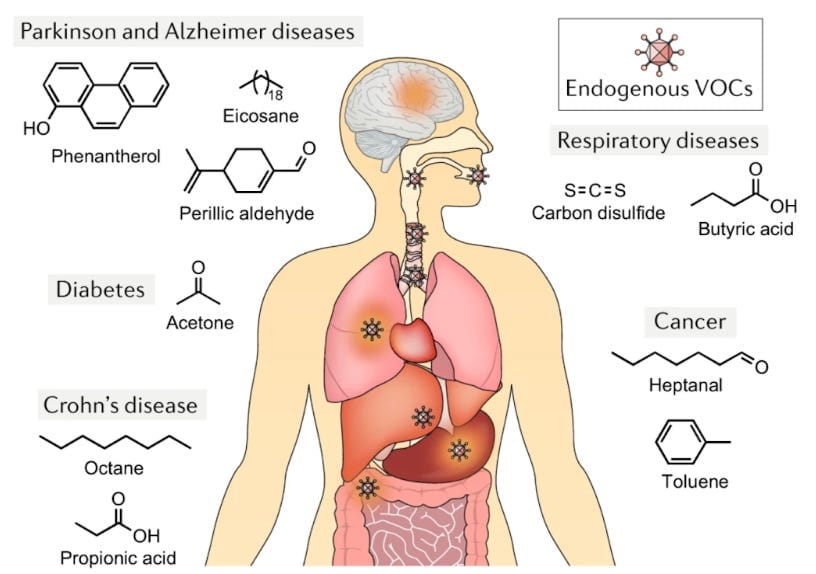
Figure 3. Distinct diseases are associated with characteristic VOC signatures emitted through breath, skin, and sweat, reflecting underlying metabolic and pathological processes. “Induced Volatolomics of Pathologies”
Metabolomics research has identified VOC patterns associated with conditions ranging from Parkinson’s to several cancers and respiratory diseases. Machine learning models trained on VOC profiles have reached striking diagnostic accuracy in early detection studies, in some cases exceeding 80-90% accuracy. While this promising technology is still maturing, academic labs, startups, and biotech companies are racing to develop sensors and analytical methods capable of detecting VOC patterns and translating this emerging biochemical data into meaningful health insights.
If this biochemical layer converges with ambient sensing within medical superintelligence systems, health will be understood at a far finer resolution. This shift could unlock deeper insight into the complexities of health and aging, enable earlier intervention, and create genuine opportunities to influence disease trajectories. At the same time, it raises profound questions about how much of ourselves can be inferred from data increasingly embedded in our everyday environments.
As these technologies mature, they generate a powerful new class of personal information with no legal framework to govern its use, monetization, or protection. Most wearables still fall outside HIPAA, even though their outputs increasingly resemble clinical data. Ambient sensing and VOC analysis extend even further into unregulated territory, capturing health-adjacent information that sits between consumer product and medical signal.
At the same time, this shift opens the door for observation and intervention to happen in parallel, grounding clinical insight in dynamic physiology rather than episodic encounters. This has particular significance for populations that have historically been underrepresented in clinical research, where continuous, real-world data can surface patterns traditional trials often miss.
Regulation, restraint, and democratization have historically been shaped by those with the most institutional or political leverage. But this next horizon of healthcare will be built on our data, which means the public has both the standing and the responsibility to stay engaged. That starts with paying attention to how health-relevant technologies are governed: following the FDA’s evolving guidance on general wellness and clinical decision support, participating in public comment when new frameworks are proposed, and understanding how health data and AI are regulated at the state level, where much of the real tension is likely to play out. Medical superintelligence will not be defined by any single law or institution, but by the collective decisions of regulators, technologists, healthcare systems, and the public. Staying informed is not optional. It is part of how we ensure this intelligence serves the public, not just established systems of power.
Thanks for reading The Byte!
The Byte is The AI Collective’s insight series highlighting non-obvious AI trends and the people uncovering them, curated by Noah Frank and Josh Evans. Questions or pitches: [email protected].
Our Premier Partner: Roam

Roam is the virtual workspace our team relies on to stay connected across time zones. It makes collaboration feel natural with shared spaces, private rooms, and built-in AI tools.
Roam’s focus on human-centered collaboration is why they’re our Premier Partner, supporting our mission to connect the builders and leaders shaping the future of AI.
Experience Roam yourself with a free 14-day trial!
➡️ Before You Go
Partner With Us
Launching a new product or hosting an event? Put your work in front of our global audience of builders, founders, and operators — we feature select products and announcements that offer real value to our readers.
👉 To be featured or sponsor a placement, reach out to our team.
The AI Collective is driven by our team of passionate volunteers. All proceeds fund future programs for the benefit of our members.
Are you subscribed across our platforms? Stay close to the community:
💬 Slack: AI Collective
𝕏 Twitter / X: @_AI_Collective
🧑💼 LinkedIn: The AI Collective
📸 Instagram: @_AI_Collective
About Audrey Kennedy
Audrey Kennedy is an R&D scientist at the intersection of chemistry, fragrance innovation, and AI-driven product development. At Osmo, she built and scaled technical workflows that connected perfumery, analytical chemistry, and machine learning, translating volatile signals into structured data and applied systems. Her work focused on turning invisible chemical information into meaningful sensory and product outcomes.
About Kiran Suryadevara
Kiran Suryadevara is a clinician-technologist and founder of Xogenous Labs, a strategy and research studio focused on healthcare, technology, and systems design. She leads early-stage strategy across digital health and social impact initiatives, translating complex scientific and regulatory landscapes into practical models. Her work centers on aligning policy, product, and public interest in emerging health systems.